Research & Publications > The Hong Kong Practitioner > Clinical Quiz

Clinical Quiz (Please login 'Member Area' for online submission of latest issue)
Clinical Quiz December 2023
A 68-year-old man presented with pigmented ‘mole’ over left nostril
Sze-man Wong
|
Readers are invited to participate in the Clinical Quiz*. Simply answer the question, fill in the reply slip and return it to the College by 19 February 2024. Each reader is allowed to submit one entry only. The name of the winner and the answer will be published in the March 2024 issue.
*Note: There would be no prize award for this issue while sponsorship for Clinical Quiz has been ended in September 2020 issue. The answer of the Clinical Quiz for this issue will be announced in the next issue. Thank you for your support.
|
Clinical history:
A 68- year-old man presented with pigmented ‘mole’ over left nostril. He recalled that there was a black-coloured pin-head size ‘mole’ over left nostril 3 years ago which gradually increase in size and occasionally bleeding after scratching.
What is likely diagnosis?
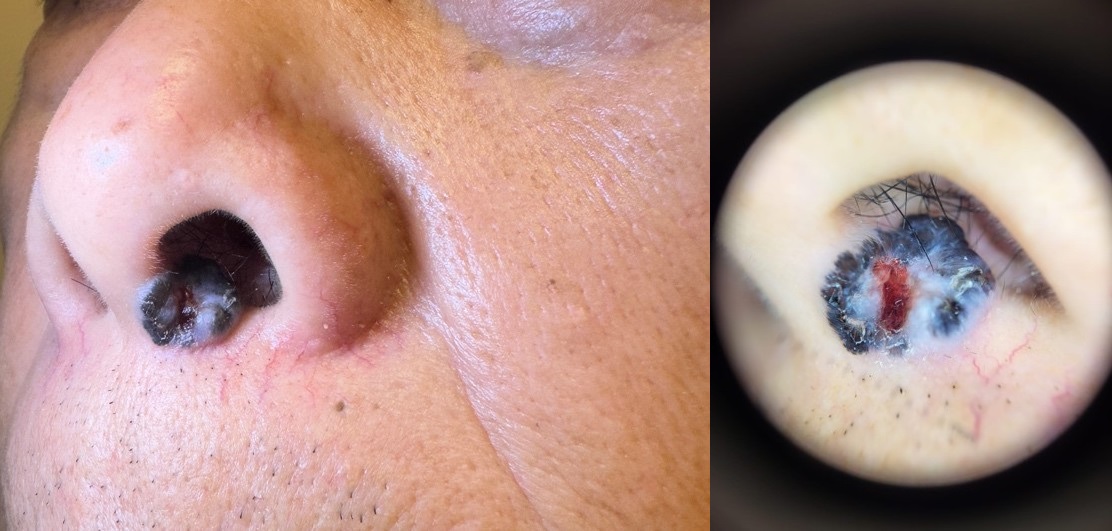
| A. | Malignant melanoma |
| B. | Squamous cell carcinoma |
| C. | Basal cell carcinoma |
| D. | Angiosarcoma |
Answer:
C. Basal cell carcinoma
The most likely clinical diagnosis is basal cell carcinoma. Clinically, the salient features include pearlcoloured, rolled border nodule, with central crater ulceration and arborising blood vessels.
General pointers to skin malignancy includes those rapid change in size, non-healing ulcer and bleeding and increase in pigmentation. BCC is typically slowgrowing. Other differential diagnoses include malignant melanoma, squamous cell carcinoma and angiosarcoma.
Basal cell carcinoma (BCC) is a non-melanoma skin cancer formed by uncontrolled growth and replication of basal cells in the lower levels of the epidermis. A BCC is sometimes referred to as a rodent ulcer and is among the most commonly diagnosed skin cancer worldwide, accounting for 65 - 75% of skin cancers.
BCC is more common in individuals with previous history of skin cancer, repeated episodes of sunburn, outdoor occupation or recreation, particularly during childhood. It is also more common in individuals with inherited genetic predisposition such as Gorlin syndrome, or xeroderma pigmentosum, or family history of skin cancer, or other risk factors such as arsenic exposure and irradiation or immunosuppressive state secondary to medications/ disorder e.g. post organ transplantation.
The clinical subtypes of BCC include superficial BCC, morpheic BCC, and nodular BCC. The diagnosis of BCC in individuals with darker skin types, such as Asians, Indians, Hispanic, can be difficult due to its rarity and pigmentation. More than 50% of BCCs found in Asians or non-fair skin types are pigmented with a ‘pearly’ brown or black appearance.
Nodular BCCs are the predominant subtype found in skin of colour or Asians as in this case. As it is usually slow-growing, small pigmented BCC can be neglected as ‘mole’ lesion in elderly, who might seek medical help only after the lesion getting bigger in size, become oozing or ulcerated.
Skin biopsy is required and essential for definitive diagnosis.
For those superficial and thin nodular BCC, the first-line treatment is complete excision.
Alternative approaches such as curettage, electrocautery, cryotherapy, laser ablation may be considered in patients with low-risk superficial BCC. Other non-surgical treatment includes topical 5% imiquimod, topical 5% fluorouracil, radiotherapy and photodynamic therapy. These treatment modalities may be considered in elderly patients not keen for aggressive surgical treatment and understanding of the risk.
However, for those high-risk BCC, recurrent BCC and BCC in critical anatomical sites such as over the central face, microscopically controlled surgery (Mohs’surgery) shall be offered.
Moreover, in patients with locally advanced and metastatic BCCs, systemic hedgehog inhibitors such as vismodegib shall be considered.
The slide and the question were prepared by:
Dr. Sze-man Wong, MBBS, MRCP(UK), MSc(London), FHKCP, FHKAM, FRCP(Edin)
Consultant,
Division of Dermatology, Department of Medicine, Queen Mary Hospital, Hong Kong SAR
Back
